Neurointerventional Radiology
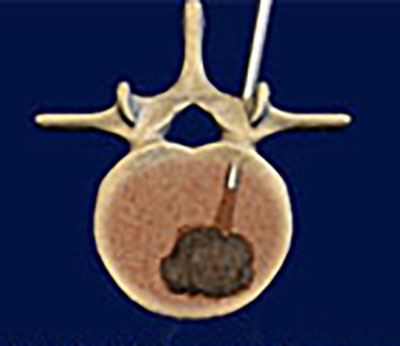
Neurointerventional Radiology (also known as Neurointerventional Surgery or Endovascular Neurosurgery) is a specialty that performs minimally invasive procedures to diagnose and treat diseases of the brain, neck, and spine. Interventional procedures use state-of-the-art image-guided techniques to deliver treatments through a small puncture in the skin (percutaneous route) instead of open surgery.EXPERIENCE MATTERS
CRL’s Neurointerventional Radiology Section, also known as the “MN Brain Docs,” is a highly-skilled team of physicians that use the most advanced techniques to treat some of the most complex neurological diseases. They are supported by specialized neurointerventional nurse practitioners with many years of experience in neurology and neurosurgery. The practice has treated over 3,000 intracranial aneurysms endovascularly, one of the highest volumes in the nation.
COLLABORATIVE CARE
The practice is located in the Neuroscience Institute at Abbott Northwestern Hospital, the leading center for neurological care in the Twin Cities and Upper Midwest. The Interventional Neuroradiology practice works closely with highly experienced neurosurgeons, neurologists, neuro-oncologists, intensivists, interventionalists, and otolaryngologists to provide complete neurological care.
FOCUSED ON QUALITY AND INNOVATION
CRL’s Neurointerventional Radiology practice is at the forefront of innovation in the field, being highly involved in new device trials, outcomes research and the development of new technologies. These activities also foster a culture of safety and continuous quality improvements in patient care.